|
We want to preserve the little energy that they're able to give us. Gradual progression of the activities, prevent overexertion. Remember, we want to make sure that we're going to do some range of motion exercises, and then we'll increase those from sitting then standing. So, we are going to gradually increase activity as tolerated. In one week, we have to gradually increase their activity. We want to condition them to tolerate activity, but we can't go from zero to 100. 
So we want these patients to be conditioned. The next thing we want to do is we want to gradually increase activity. It allows for the heart rate and breathing to normalize. Remember rest periods allow a patient to conserve energy. We want to give the patient enough time to take those grueling activities. It's very important for us as nurses to coordinate with the patient, we want to coordinate rest periods. And if that is the case, we want to make sure that we stop the activity and we administer any supplemental o2 that they need. Um, some patients will also see a decrease in their o2 saturations. They may also have increased blood pressure. 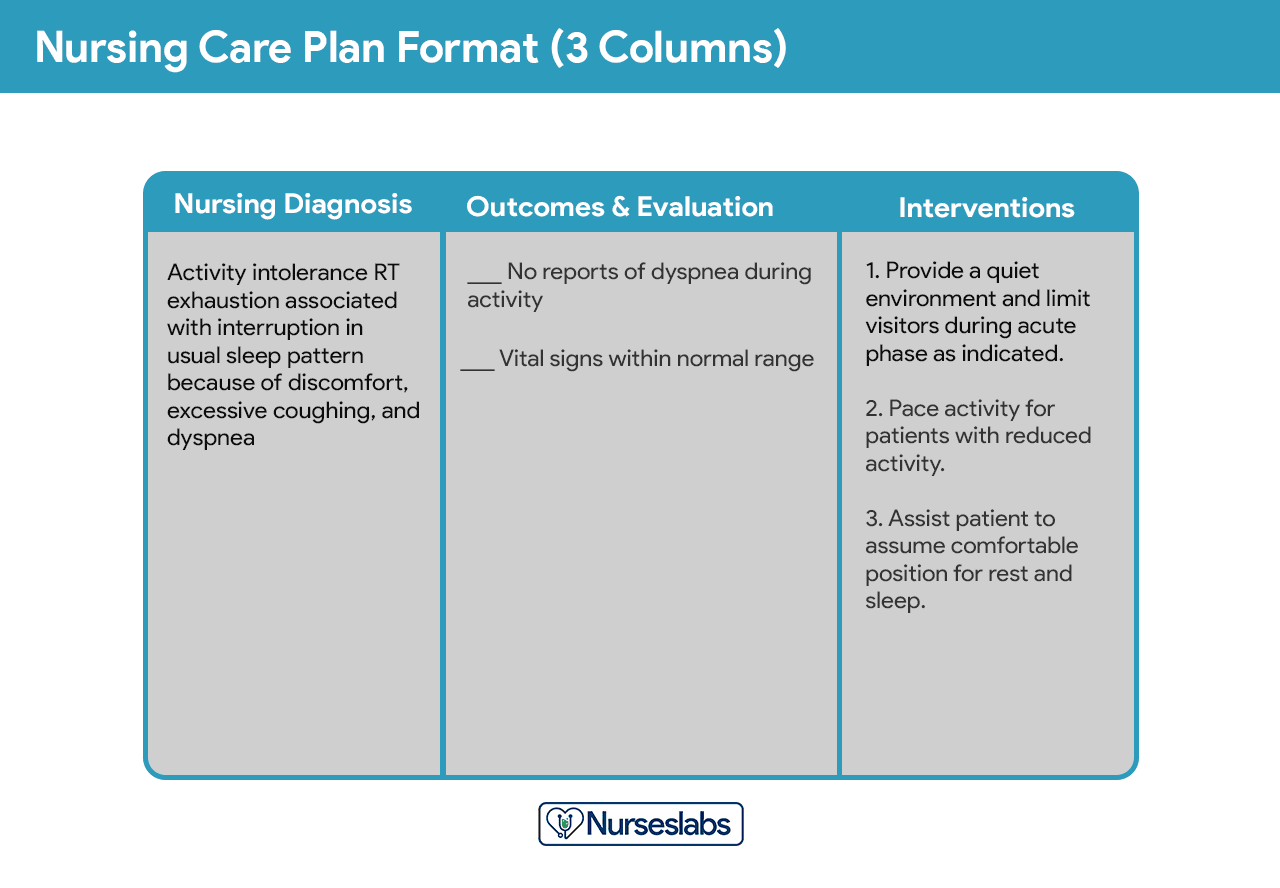
That's going to be in relation to any activity that they have. Some of the vital signs we may see on the monitor again, is increased heart rate. Remember this person looks like a patient in heart failure. The next thing is we want to monitor their vital signs. Remember we always want to assess to gather our data. These are the reasons why a person would have activity intolerance, respiratory conditions, such as COPD, or Asthma can also contribute to this activity tolerance. Um, they can also have a low ejection fraction. So what are we going to do? What are interventions that we're going to do with this patient? Well, the first thing is we're going to get us a good cardiac and a good respiratory assessment. They may also have some edema and they're going to have, uh, some dysrhythmias. So walking down the hall, if they walk too far too fast, they're going to have that tachycardia. Some of those things that mimic heart failure are, they are going to have an increased heart rate, increased blood pressure, and that's going to be in response to activity. These patients are going to have signs of heart failure. So, the first thing we're going to notice with our objective data is we are going to notice that they have signs of heart failure. Now, when we observe these patients, there's going to be a few things that we see once again, it's going to mimic heart failure. Again, they may complain of some chest pain and weakness. Again, it doesn't take much exertion, but when they exert themselves, they are typically very short of breath. They also have some dyspnea or shortness of breath on exertion. Um, very minimal or small activities, kind of take all of their energy. So, some of the things that they are going to, uh, let us know the subjective data is, they are going to complain of some fatigue. So, the patient with activity intolerance is someone who is going to come in very similar to someone looking like a heart failure patient. The patient will also report an increase in activity tolerance. 
The desired outcome is that the patient is going to, uh, demonstrate the ability to participate in normal life activities with decreased occurrence of dyspnea, chest pain, diaphoresis, dizziness, and changes in vital signs. We want to obtain an EKG for cardiac involvement, and we may need to refer the patient to a cardiologist. We want to assess the respiratory and cardiac status. Some nursing considerations that we want to keep in mind are that we want to monitor vital signs. A contributing factor is often tissue hypoxia caused by decreased cardiac output. Activity Intolerance is a common side effect of heart failure and can be related to generalized weakness and difficulty resting and sleeping. Activity tolerance is the insufficient, physiological or psychological energy to continue or complete necessary or desired tasks. This is the nursing care plan for activity intolerance.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
